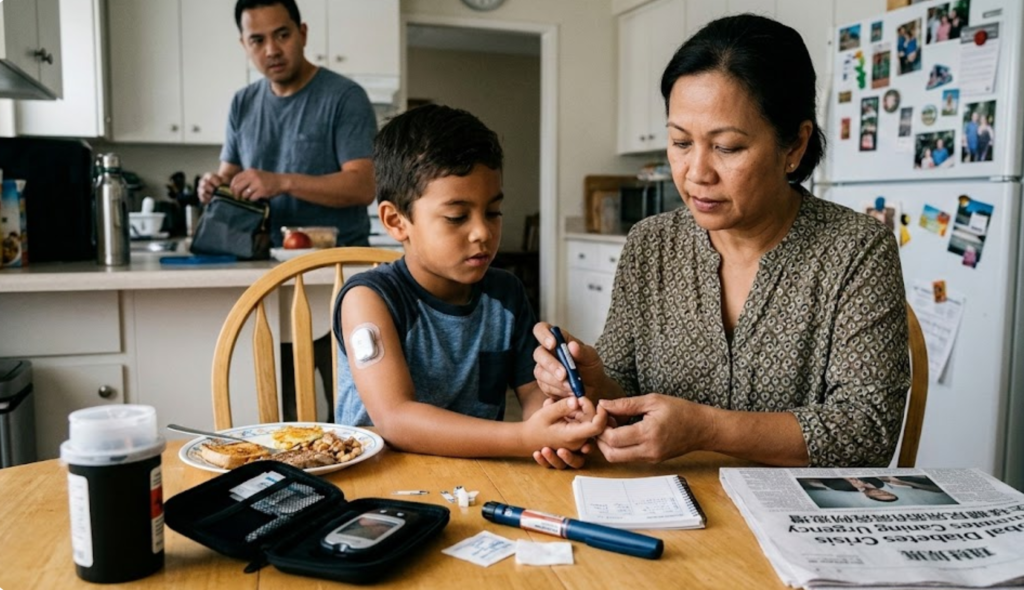
Our exploration in the field of T2DM
Existing problems
Among chronic diseases, diabetes has become the disease with the highest incidence in recent years, and diabetes is one of the most important chronic non-communicable diseases in the world. More and more serious, diabetes and its complications seriously affect the quality of human life. Especially with the changes in dietary structure and living habits, the incidence of diabetes has increased year by year, and it has become a frequently-occurring and common disease.
The harm of diabetes is not only due to the disorder of energy metabolism, the patient suffers from blood sugar out of control, but also the irreversible damage to the eyes, kidneys, nerves, blood vessels and other organs caused by various complications after the disease, and the patient’s body and mind are greatly affected. Destruction. In severe cases, diabetes and various complications directly threaten life. According to recent statistics from the International Diabetes Federation (IDF), the lifetime incidence of diabetes has approached 10%, and is rapidly increasing at a double-digit percentage every year. Faced with the “diabetes in every family, everyone is at risk” situation. Therefore, how to treat diabetes and implement long-term health monitoring for people susceptible to diabetes has become one of the most serious challenges in the medical field.
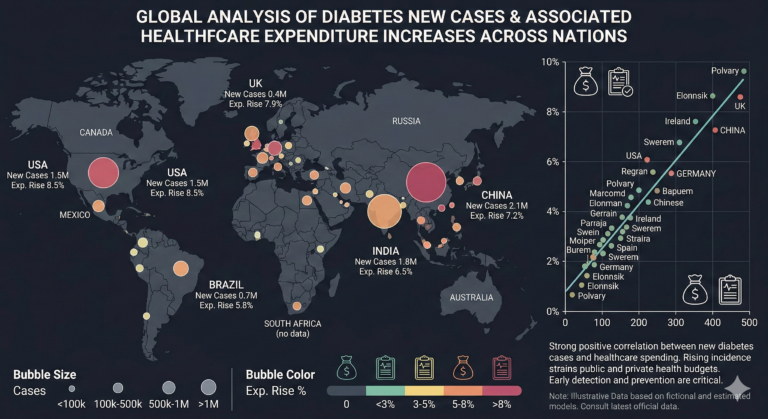
there is a strong positive correlation globally between new diabetes cases and healthcare expenditure increases, placing a severe financial strain on national health insurance systems; for instance, China (2.1M new cases, 7.2% expenditure rise) faces massive volume-based pressures, while the USA experiences the highest spending spike at 8.5% despite fewer cases (1.5M), highlighting the urgent need to prioritize early detection and preventative care to alleviate the escalating burden on public and private health budgets.
AI & personalized medical solutions
With the development of medical research, it is now found that diabetes is a disease caused by the interaction of genes and the environment, in which genetic genes determine the occurrence and development of 60% of diabetes, including the etiology, course characteristics, and complications.
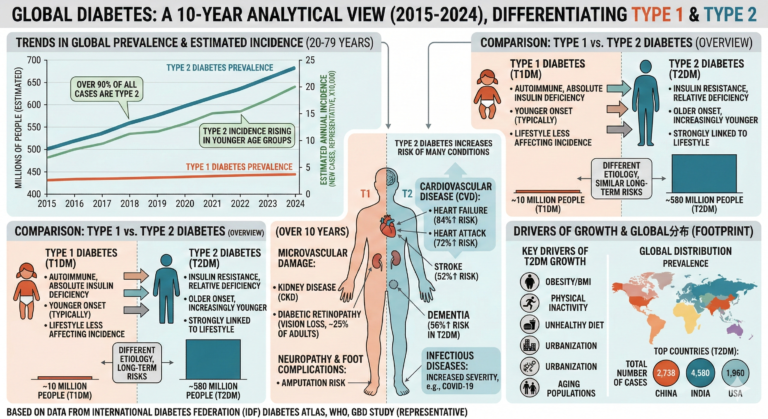
After years of efforts by the global medical community, the understanding of diabetes has long since changed. The pathogenesis, related genes and environmental factors of diabetes have been fully studied, and a series of important conclusions have been obtained. Extensive data indicate that, in addition to the well-known “type 1, type 2” classification of diabetes, diabetes can be divided into multiple subtypes based on pathogenesis. For example, type 1 diabetes can be further divided into 1A and 1B according to autoimmune markers; type 2 diabetes can be divided into insulin resistance and relative insulin deficiency, and the severity needs to be further divided according to B cell destruction. degree, increased hepatic glycogen output, etc. At present, ADA (American Diabetes Association) has published 56 types of diabetes classification, and the number is constantly increasing. Therefore, it is currently recognized internationally that diabetes is a syndrome (a general term for many similar diseases), rather than a single disease.
If we combine AI with precision medicine for diabetes, patients can benefit from improved diabetes health management.
AI models can be used to mine data from diabetic patients and enable personalized medication management.
There are nearly 20 kinds of hypoglycemic drugs. However, in general, due to the urgency of diabetes, diabetic patients seldom try to change their medicines actively, but tend to use first-line medicines with certain effects for a long time, or common medicines covered by medical insurance. However, these drugs are likely to be suboptimal or even have high side-effects, thus delaying the course of the disease.
The most widely used drug for diabetic patients, as an example. Metformin is almost the only first-line drug recommended in the guidelines of various societies, and it has also been shown to be effective. But now there are many clinical cases of metformin ineffective or intolerable. At present, a number of studies have found that mutations in the gene ATM locus are significantly related to the efficacy of metformin, while the OCT1 gene is significantly related to its plasma concentration. Therefore, as long as we detect these sites, we can predict whether the patient is suitable for the drug before taking the drug, and we don’t have to make the patient detour.
Using AI for personalized management to prevent diabetes complications
Because diabetes complications have strong genetic correlations, we can evaluate common complications of diabetes through genetic means, so as to carry out targeted prevention. Complications that can currently be predicted through genetic and big data information include: eye disease, extremity disease, kidney disease, cardiovascular disease, and neurological disease.
Using AI to reduce doctors’ workload
Without AI, it would be difficult for a doctor to manage multiple diabetic patients simultaneously. AI assistants can help doctors reduce their workload, and in the future, patient management could be automated.